No, Chiropractic Adjustments Do Not Cause “Toxic Release” Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief “Toxins” is a vague word that doesn’t really mean anything. Chiropractic adjustments greatly improve your body’s natural healing abilities, but there is not a specific toxin release that will make you feel sicker or healthier after an adjustment. Chiropractic care corrects spinal misalignment and subluxations, leading to a stronger nervous system and improved overall health. Chiropractic care does not correct body toxicity , which is a vague and dubious concept in the first place. However, chiropractic adjustment may strengthen the nervous system’s communication with the liver or kidneys, which both naturally detoxify the body. Strengthening these detoxing organs may help get rid of toxins, such as ammonia and uric acid. If your chiropractor employs a lot of massage techniques, that muscle fiber activation may lead to some temporary dehydration, which can lead to a slight feeling of illness if you don’t hydrate well afterwards. When I’m seeing patients, I’m honest with them. I’m a chiropractor, not a new age detox guru. Upper cervical chiropractic already heals people in surprising, evidence-based ways. Toxin release is unnecessary for the healing process, and I doubt it’s actually a thing. If you want a chiropractor who will be honest with you while using conservative, non-pharmaceutical treatments when possible, schedule your appointment with me at Denver Upper Cervical Chiropractic today. You can call us at 303-955-8270 . What Are “Toxins,” Anyway? Toxins are harmful substances that can make you sick in a variety of ways. However, the word “toxin” is so vague and all-encompassing that it loses all meaning when cited by many “health” influencers. In theory, releasing toxins through chiropractic adjustment or other means can make you feel groggy in the short-term then healthier in the long-term. I disagree with this theory — it’s not based on observable, definable, replicable research. Here’s a list of “toxins” that many chiropractors claim can released by chiropractic care: Polychlorinated biphenyls (PCBs) Chlorofluorocarbons (CFCs) Histamine Lactic acid Artificial preservatives Inorganic pesticides Industrial chemicals Heavy metals Air pollutants Do chiropractic adjustments really release toxins? No, chiropractic adjustments don’t really release toxins. Some claim the crack in your back is toxic release, which is untrue. I share the list above so you can do your own research — scientific study does not support the idea that any of those compounds are “released” by chiropractic adjustments or any form of spinal manipulation. In fact, if something leaks from your spinal cord, you probably need to visit an emergency room — because that something is spinal fluid, and you have an injury. Scientific Evidence for Body Toxicity The scientific evidence for “body toxicity” is next to none. In my educated opinion, the few instances of body toxins that could actually make you sick would benefit from using the specific toxin’s name, not the vague term “toxin.” It’s likely true that your body is exposed to various chemical compounds in your everyday life that make your body less healthy. However, every person is different, and every toxin is different. Calling them all “toxins” is unhelpful and medically meaningless. Chiropractic care improves your whole body health by correcting spinal misalignment , which strengthens your nervous system and even treats many kinds of headaches. But chiropractic adjustments don’t directly release toxins. Endotoxemia is a measurable variety of body toxicity which may warrant further research. Diet-induced systemic bacterial endotoxemia may result from consuming high amounts of sugar, flour, and oils. Healthy diet and healthy lifestyle can prevent endotoxemia. You May Feel “Sick” After an Adjustment Most people don’t feel “sick” after an adjustment, but some report fatigue and soreness. These symptoms are uncommon but natural and temporary, requiring a short adjustment period. Why does my body feel weird after a chiropractic adjustment? If your body feels lightheaded after a chiropractic adjustment, it’s probably due to a large change in the stimulus from proprioceptors and your body recalibrating to the new position of the corrected spine. In my experience, chiropractic patients don’t feel sick after an adjustment. If the rare occurrence they feel sore, lightheaded, or fatigued, it certainly has nothing to do with toxins. What are the symptoms of toxic release after chiropractic adjustment ? According to some, the side effects of toxic release after a chiropractic adjustment may include: Headache Fever Fatigue Nausea Dizziness Night sweats Sore or tight muscles Abdominal distress Flu-like symptoms What About Feeling Sick after Massage Therapy and Exercise? I’ve had patients ask about the ill feeling they sometimes have after massage or exercise, suggesting this is the same thing they feel after getting adjusted. Exercise can make you sweat, which is one of your body’s built-in detoxification processes. Massage, however, just dehydrates you (which can cause that ill feeling). During massage therapy, patients experience relaxation, but not release of toxins. You can actually get dehydrated due to your connective tissue and muscle fibers being activated and exercised, drawing moisture from your body and dehydrating you from the inside. This is why massage therapists give you water and tell you to drink more than normal after your appointment. During exercise, sweat naturally gets rid of some toxins and waste products. Physical exertion also pumps the blood circulation, accelerating detoxification in the lymph nodes and kidneys. A 2022 study found that more heavy metal toxins were released in sweat after exercising versus sweat from a heat sauna, implying that sweat alone is not the answer. Visit a Chiropractor Who Uses Only Evidence-Based Treatments I’m Dr. Ty Carzoli, an upper cervical chiropractor who has helped hundreds of patients overcome back pain , neck pain, migraines , headaches , vertigo, range of motion, and even mental health conditions. I don’t do these through the nebulous practice of so-called “toxic release,” but through evidence-based chiropractic treatment. Find a chiropractor who uses techniques that will actually help with the concerns you have. Any healthcare clinician you see should be able to defend or explain their rationale with evidence and sound reasoning, not appeals to emotion, metaphysical explanations, or ambiguous and vague jargon. Take control of your whole-body well-being , and work with us on a treatment plan that works for your unique situation. Schedule your appointment with Denver Upper Cervical Chiropractic right away. We are open on Friday but reserve that
What Is Orthospinology? Benefits, History, What to Expect & More
What Is Orthospinology? Benefits, History, What to Expect & More Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief Orthospinology is a subspecialty of chiropractic healthcare targeted to the top two vertebrae of the spine. Fixing misalignments in your upper cervical spine may address many underlying health problems , including seizures, chronic migraine, Parkinson’s disease, multiple sclerosis, high blood pressure, and more. At Denver Upper Cervical Chiropractic , we employ the evidence-based techniques of orthospinology to bring relief to patients who have found little success with man-made medications or want to avoid invasive surgeries. Listen to real customer testimonials about how upper cervical chiropractic care worked for them. Read below for more on orthospinology, including what it treats and what to expect from a visit to your qualified orthospinology chiropractor. What is orthospinology? Orthospinology is a gentle chiropractic technique that aligns the upper cervical spine (top two vertebrae) to reduce pain, promote overall wellness, and relieve chronic health conditions. Orthospinology is a conservative alternative to pharmaceuticals or surgery. This subspecialty of chiropractic care focuses on the upper cervical spine, which consists of the upper 2 vertebrae: The atlas , or C1 The axis , or C2 Upper cervical chiropractic care is gentle, not rough. We are not trying to ‘crack your back;’ we are fixing how your upper spinal cord communicates with your brain stem. This is what sets orthospinology apart from other chiropractic care. Orthospinology vs. NUCCA vs. Atlas Orthogonal National Upper Cervical Chiropractic Association (NUCCA) defines and regulates the practice of manually adjusting the upper cervical vertebrae based on x-ray analysis. This practice is slightly different from orthospinology. What is the difference between NUCCA and Orthospinology ? NUCCA adjustments are usually done by hand, but orthospinology procedures use instruments. A patient with good outcomes at a NUCCA office will typically have good outcomes at an orthospinology practice, and vice versa. Atlas Orthogonal is a little different from orthospinology though they are both upper cervical low-force procedures. The Atlas Orthogonal technique looks much like an orthospinology adjustment, but the instrument delivers the adjustment with a “percussive force” — essentially, a sound wave. Orthospinology techniques utilize a similar percussive instrument for some types of misalignments, but a larger table mounted instrument with a mechanical excursion for more. History of Orthospinology In the 1940s, Dr. John F. Grostic developed the Grostic technique — the beginnings of orthospinology. The Grostic technique focused on optimizing: Analysis specificity — making sure diagnostics accurately identify the underlying problem Adjustment precision — making sure chiropractic treatment precisely targets the underlying problem In the 1970s, Dr. John D. Grostic continued his father’s research. He expanded the list of upper spinal misalignment’s adverse effects on the central nervous system, based on overwhelming evidence. Orthospinology was born from the Grostic technique. Clinicians sought to improve the reproducibility of adjustments while minimizing human error with gentle, precise instruments. What causes neck misalignment? The following events may cause neck misalignment: Poor posture, including during sleep or work Traumatic spine or head injury (sports injuries, motor vehicle accidents, falls) Repeated “minor” injuries to the spine (chronically wrong lifting, staring down at phones) A long, stressful labor What causes atlas subluxation ? Traumatic injury is usually what leads to Atlas Subluxation Complex — a subluxation in your top vertebra. Poor posture and repeated injuries are common risk factors that worsen atlas subluxation. What happens when C2 is out of alignment? When the C2 (axis) is out of alignment, you can expect pain, numbness, weakness, or even loss of bladder/bowel control. You should seek upper cervical chiropractic care to correct C2 misalignment and avoid chronic health problems or long-term complications. What to Expect During Orthospinology Treatment During the orthospinology treatment process, expect an initial consultation. On your first visit , upper cervical chiropractors may not administer an adjustment. Precise analysis and diagnostics are crucial to orthospinology, so chiropractors often take a few days to process results. At your initial consultation, your upper cervical chiropractor may do a physical exam, digital x-ray analysis, maybe even a cognitive exam. On your second visit , chiropractors will typically perform the first adjustment. Upper cervical adjustments are gentle. Forget about those rough twists and cracks. Orthospinology is gentle enough for children and grandmas alike. These adjustments are often instrument-assisted. Sometimes, the instruments will be handheld. Other times, the instruments are mounted on advanced equipment.This video helps you know what to expect from an orthospinology adjustment. https://vimeo.com/299982455?fl=pl&fe=shhttps://youtu.be/MtWUoA5tt-8?si=GoG2atiI-DyQ0uga At Denver Upper Cervical Chiropractic, we also have a post-adjustment room for patients to relax and cool down after spinal realignment. Our calming post-adjustment room contains: Zero-gravity chairs Weighted blankets Noise-canceling headphones with binaural beats Essential oil diffuser Gentle lighting In our offices, we may also recommend upper and lower back stretches to help with certain conditions. How long does it take to realign your spine? It takes one adjustment to start realigning your spine. The total number of visits needed for total realignment varies by case and depends on the condition of the patient. However, a handful of visits to your chiropractor every year are likely needed to maintain spinal alignment. The Orthospinology Technique: Before and After Spinal decompression therapy is typically not recommended for the following people: Before After Before-After These before and after pictures from www.orthospinology.org show an average individual and how misaligned their spine may be before a spinal correction. Another method upper cervical chiropractors use is analyzing functional leg length by comparing the patient’s heels before and after adjustments. Before After Benefits of Orthospinology Orthospinology aims to improve nervous system function, immune system function, body imbalance, and overall wellness. But what specifically do upper cervical procedures treat? According to peer-reviewed research and case studies, the possible benefits of orthospinology /upper cervical care include improving medical conditions such as: Lower back pain Neck pain Knee pain Headaches and migraines Seizures Scoliosis Fibromyalgia Multiple sclerosis Parkinson’s symptoms Bowel dysfunction Asthma Low blood pressure High blood pressure Immune dysfunction (including when related to HIV ) Tourette’s syndrome Cerebral palsy Autism spectrum disorder Orthospinology as a Subspecialty of Chiropractic Orthospinology is a subspecialty of the chiropractic profession. It takes many credit hours of additional education and certification before
The Atlas Bone & When You Might Need an Adjustment
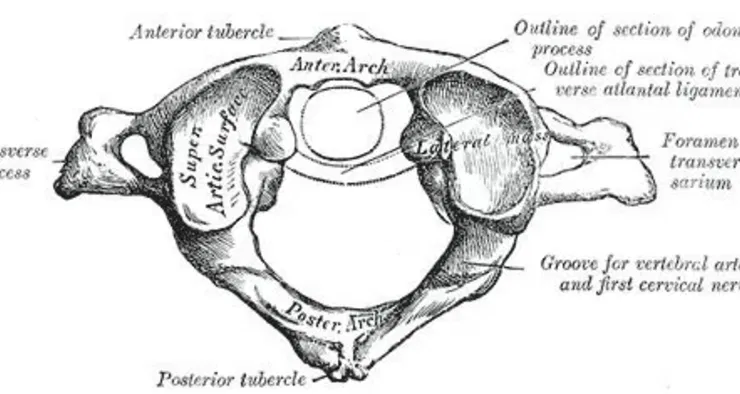
The Atlas Bone & When You Might Need an Adjustment Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief Much like the Atlas in Greek mythology who supported the entire world, the function of the atlas bone is critical: it supports your entire head. The atlas bone (C1) connects your skull to your spine, and — with the support of the axis vertebra (C2) just below — the atlas determines your head’s full range of motion. Misalignments in the atlas bone can cause chronic pain, stress, decreased range of motion, and tension in the head or neck. Keep reading to understand this critical vertebra and determine when a misaligned atlas may be causing you issues. From Anatomy, Head and Neck: Cervical Vertebrae (Public Domain) What Is the Atlas Bone? The atlas bone is the top bone or first cervical vertebra connecting your skull to your spine. It’s also known as the C1 vertebra in your cervical spine . Your whole spine has 7 cervical vertebrae that connect to the 12 thoracic vertebrae, which connect to your 5 lumbar vertebrae. Those lowest 5 vertebrae make up the lumbar spine and connect to the sacrum, then the coccyx at the base of your spine. Uniquely among vertebrae, the atlas vertebra at the very top of your spine lacks a vertebral body, spinous process, and the intervertebral discs found elsewhere in the spinal column. The atlas is a ring-like structure that joins the occipital bone above it with the axis, or C2 vertebra, below it — thanks to both the atlantooccipital joint and the atlantoaxial joint. These joints belong to a class of synovial joints that act as pivot points in the body. In this case, the pivot is your head movements. How does the atlas bone affect overall health? A misaligned atlas bone directly impacts headaches, migraines, neck pain, range of motion, and balance. A dysfunctional atlas may indirectly contribute to chronic pain, inflammation, brain fog, and mental health problems. Let’s dive into the atlas bone’s support structure and general anatomy to get a deeper understanding of how it works. Here are the major parts of your atlas bone: Lateral masses Transverse process Anterior arch Posterior arch Vertebral foramen Lateral Masses The lateral masses (Massa lateralis atlantis) of the atlas bone are its thickest and sturdiest parts, which is by design. The pair of masses support the weight of your skull. Superior and inferior facets, or small joints, are found on each side of the lateral masses. The superior articular facets on the superior surface connect to the occipital condyles on your occipital bone. These structures allow for neck flexion and nodding movements of the head. This part of your atlas allows you to nod your head “yes” — why the atlas is also called the “yes bone.” The inferior articular facets on the inferior articular surface allow articulation with the axis, or second cervical vertebra, and head rotations. Essentially, these facets are where the two joints meet. Transverse Processes The transverse processes are large projections from the lateral masses that attach to the muscles here and help you rotate your head and neck. These muscles include the rectus capitis lateralis, a small muscle important to lateral bending of the occiput, or the back of your head. The transverse foramen in the transverse processes is a hole for your vertebral artery. From Anatomy, Head and Neck: Atlantoaxial Joint (© 2024, StatPearls Publishing LLC) Anterior Arch The anterior arch is concave on one side and convex on the other. That shape allows it to work as a connecting segment for the odontoid process (dens) of the axis below and the transverse ligament. From above, it attaches the long muscle of the neck (longus colli muscles) with the anterior tubercle. The upper border of the anterior arch attaches to the anterior atlantooccipital membrane. The lower border attaches to the anterior atlantoaxial ligament and the anterior longitudinal ligament. Most importantly, these connections are a pivot point with the axis. Posterior Arch The thin posterior arch that ends behind the posterior tubercle makes up about two-fifths of the circumference of the atlas ring. The posterior tubercle sits at the apex of the posterior arch and serves as an attachment site for the nuchal ligament (ligamentum nuchae), which spans the 7 vertebrae of the cervical spine. A groove in the posterior arch allows the vertebral artery to pass through here and the foramen magnum and continue along the spinal column. Defects in this area that lead to interference between the atlas and your skull can cause neurological problems down the line if left untreated. Vertebral Foramen The vertebral foramen is a large opening in the bone for both the spinal cord and the odontoid process of the axis. On the axis side, it serves as the start of a pivot point for your C2 vertebra. Read Next: Trigeminal Neuralgia vs TMJ, What Are They? Atlas Misalignment Atlas misalignment may cause various health problems and impact the structural integrity of your spine over time. How does your atlas get misaligned? Your atlas can get misaligned due to injury, abnormalities in your bone structure , or a variety of conditions affecting the spine and musculoskeletal system. Poor posture can also cause atlas misalignment over time. One rare injury that directly affects the atlas is a Jefferson fracture, most often seen alongside spine or head injuries. Generally, atlas fractures are more common in the elderly. It can be difficult to know how many people have an atlas misalignment, as many patients don’t seek care immediately. Atlas misalignment is among the most common conditions addressed by chiropractic care. What are the symptoms of a misaligned atlas? The symptoms of a misaligned atlas include: Headaches Migraines Pain in the jaw, neck, and back, and muscle stiffness Hearing problems, e.g. tinnitus, hearing loss, inner ear conditions Shoulder pain or misalignment of the scapulae, or shoulder blade Restricted movement of the head up and down or side to side Dizziness, including vertigo Balance problems Difficulties with coordination and concentration Muscle spasms Pelvic and hip misalignment Trigeminal neuralgia
Spinal Decompression Therapy: Heal the Spine Naturally
Spinal Decompression Therapy: Heal the Spine Naturally Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief If you have persistent chronic pain in your back , neck , or hips, spinal decompression therapy may offer relief. This non-invasive therapy treats the root cause of your pain. This form of therapeutic traction is most helpful for people with disc degeneration, bulging or herniated discs, and radiculopathy (pain radiating into the arms or legs). Spinal decompression can help a significant percentage of patients without requiring surgery. This is especially helpful for patients with disc issues like loss of disc height that are traditionally treated with surgery alone. In our office, we’ve seen a significant improvement in pain for patients with disc problems, especially those whose spines don’t respond as quickly to chiropractic adjustments. It’s best when used over multiple sessions, and all of the feedback I’ve gotten is that it’s incredibly gentle and a great help. In fact, we invested in our own spinal decompression table just recently! Learn more about the benefits of spinal decompression below. What Is Spinal Decompression? Spinal decompression is a non-surgical therapy that may relieve back pain and promote the natural healing of the spine. Decompression therapy gently stretches the spine, creating a vacuum effect that helps retract herniated or bulging discs. It’s one of the only effective non-surgical treatment options for disc pain. A decompression table allows chiropractors greater precision in the target area, especially compared to an inversion table or other forms of traction that don’t let you dial in the tension applied or the region you’re applying tension to. This safe, painless process also enhances the flow of nutrients, oxygen, and fluids into the spinal discs, further facilitating disc healing and reducing pinched nerves. I find that patients whose spines are most stubborn to respond well to adjustments benefit most from spinal decompression. Spinal decompression should be performed by a qualified chiropractor. Do not attempt decompression at home. Your chiropractor may recommend targeted at-home stretches that are safe and helpful. “Spinal decompression” sometimes refers to surgical treatment , but non-surgical decompression therapy is not the same as surgical spinal decompression. Types of Spinal Decompression Therapy Below are the most common types of spinal decompression therapy: Motorized Traction — This method involves a traction table or similar device intermittently stretching and relaxing the spinal column. Chiropractors and physical therapists often use spinal decompression tables for the most precise results. Manual Spinal Decompression — This type is also performed by a chiropractor using instrument-free, hands-on techniques to stretch the spine. Surgery — Spinal decompression surgery may include removing vertebra bone (laminectomy) or spinal disc (discectomy). A surgeon may also fuse two vertebrae together with a bone graft. Back surgery is invasive and more dangerous than the other types but may be needed in severe circumstances. Our office at Denver Upper Cervical Chiropractic just invested in a new spinal decompression table for our patients. We are seeing incredible results in their quality of life! To schedule an appointment, call 303-955-8270. Benefits of Spinal Decompression Therapy According to recent research , the health benefits of non-surgical spinal decompression therapy include the following: Pain relief Increased range of motion More back muscle endurance Higher quality of life Fewer side effects compared to pharmaceuticals or surgery Conditions That Spinal Compression May Treat Non-surgical spinal decompression therapy may benefit these conditions: Chronic back pain Sciatica Spinal stenosis Herniated discs Degenerative disc disease Facet syndrome Symptoms of a Compressed Spine It’s vital to recognize the signs of compressed nerves and a compressed spine. If you’re experiencing any of the following symptoms, spinal decompression therapy may be beneficial for you: Chronic pain in the lower back , neck, or buttocks — Leg pain, neck pain, or back pain that doesn’t improve with conventional treatments Numbness or tingling — Sensations in the arms, hands, legs, or feet Weakness — Difficulty moving the affected parts of the body Reduced range of motion — Difficulty bending or twisting Read more: Can Chiropractors Relieve Occipital Neuralgia Pain? Common Causes of a Compressed Spine Below are the most common causes of compressed spine symptoms: Herniated or bulging discs — Discs protrude and press on spinal nerve roots when herniated or bulging Degenerative disc disease — The discs between the vertebrae lose their cushioning in this disease, leading to pain Poor posture — Posture misalignments put extra pressure on the spinal cord Back injury — Accidents, falls, and other injuries increase the risk of nerve compression and lumbar spine pain When to Discuss Surgery In certain cases, conservative treatments may fail to provide relief, and you and your doctor might consider different types of surgery. Here are the signs that orthopedic surgery should be discussed: Persistent pain — When non-invasive treatments have failed to improve your symptoms and quality of life Severe nerve damage — Evidenced by loss of sensation or weakness Loss of bowel or bladder control — Indicating cauda equina syndrome, a surgical emergency Surgery is rough on the human body and comes with side effects. Risks of surgery include: Infection Blood clots Bleeding Nerve damage Scarring Long recovery period Risks associated with anesthesia How to Prevent Spinal Compression If you prevent spine compression pain, you may not need expensive treatments. Preventing spinal compression includes adopting a holistic and proactive approach to spinal health. Below are ways to prevent spinal compression in the first place: Practice proper posture — Especially when sitting or lifting objects Regularly exercise — Strengthening the core muscles supports the spine Maintain a healthy weight — Reducing strain on the spine and back Invest in ergonomic workstations — Ensuring your work setup supports spinal health Seek professional guidance — Such as from a chiropractor or physical therapist When Spinal Decompression Is NOT Recommended Spinal decompression therapy is typically not recommended for the following people: Pregnant women Those with spine fractures or tumors Those with broken vertebrae Those who have undergone spinal fusion Those who have metal implants in their spine Those who have advanced osteoporosis Other treatments for negative pressure on spinal nerves include general chiropractic , acupuncture, and physical therapy. FAQs Is it good to decompress your spine? It is good to safely decompress your
Living in Limbo: Navigating Life with Undiagnosed Neurological Symptoms
Living in Limbo: Navigating Life with Undiagnosed Neurological Symptoms Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief The Frustration of Not Having a Diagnosis Living with undiagnosed neurological symptoms is a constant struggle, marked by a never-ending cycle of doctor visits, tests, and uncertainty. Individuals often experience symptoms that severely impact their daily lives, yet remain undiagnosed despite thorough medical evaluations. This can lead to feelings of frustration, helplessness, and even skepticism from healthcare providers. Common Unexplained Neurological Symptoms People suffering from unexplained neurological symptoms often report persistent headaches or migraines, muscle weakness or paralysis, numbness or tingling sensations, balance and coordination issues, cognitive difficulties such as memory loss or confusion, visual disturbances, and speech difficulties. Types of Unexplained Neurological Symptoms Chronic Headaches & Migraines : These can be debilitating, often occurring without an identifiable cause, leading to significant discomfort, nausea, and sensitivity to light and sound. Chronic migraines can disrupt daily life, making it difficult for individuals to maintain their regular routines. Peripheral Neuropathy: Involves damage to the peripheral nerves, causing pain, numbness, and weakness, particularly in the hands and feet. This condition can arise without a clear cause, leading to significant distress and functional impairment. Patients often describe the sensation as burning, tingling, or electric shocks. Unexplained Seizures: These can occur sporadically and are difficult to manage without a definitive diagnosis. Seizures without a known cause can be particularly challenging to treat, as they may not respond well to standard epilepsy medications. The unpredictability of these seizures adds to the patient’s anxiety and stress. Movement Disorders: Tremors, dystonia, or tics can occur without an identifiable cause, making them challenging to treat. These disorders can manifest as involuntary movements, muscle contractions, or repetitive motions, severely impacting a person’s ability to perform daily tasks. The lack of a clear diagnosis often complicates the management and treatment of these symptoms. Functional Neurological Disorder (FND): Patients experience neurological symptoms like limb weakness, seizures, or sensory disturbances without any structural or biochemical abnormalities. These symptoms can mimic serious neurological conditions but are not explained by traditional medical tests. FND can significantly impact a person’s quality of life and requires a comprehensive approach to diagnosis and treatment. Chronic Fatigue Syndrome (CFS): Characterized by extreme fatigue that does not improve with rest and cannot be explained by any underlying medical condition. Patients with CFS often experience additional symptoms such as sleep disturbances, memory issues, and muscle pain, which further complicate their condition. Autonomic Dysfunction: Involves the autonomic nervous system, leading to symptoms such as abnormal heart rate, blood pressure issues, and digestive problems. These symptoms can be severe and disruptive, occurring without a clear underlying cause. Cognitive Impairments: Includes issues with memory, attention, and executive function that are not linked to any identifiable brain injury or disease. These impairments can severely affect daily functioning and quality of life, adding to the frustration of living with undiagnosed symptoms. Sensory Disturbances: Patients may experience unexplained changes in sensation, such as numbness, tingling, or heightened sensitivity. These disturbances can affect various parts of the body and can be persistent or intermittent, complicating diagnosis and treatment. Diagnostic Challenges Exhaustive Medical History and Physical Examination: Despite thorough evaluations, a definitive diagnosis often remains elusive. Comprehensive Testing: Imaging studies (MRI and CT scans), EEGs, blood tests, and lumbar punctures frequently yield inconclusive results, adding to the frustration. The Emotional Toll The absence of a diagnosis can lead to significant emotional and psychological distress, including anxiety, depression, and a sense of isolation, as patients may feel dismissed or not taken seriously by healthcare providers. Managing Unexplained Neurological Symptoms Symptom Management Psychological Support Lifestyle Adjustments Medications such as pain relievers, antidepressants, and anticonvulsants can help manage symptoms. Pain relievers reduce discomfort, antidepressants address mood disorders and chronic pain, and anticonvulsants manage nerve pain and seizures. Physical therapy improves strength, coordination, and balance through tailored exercise programs and manual therapy techniques like massage. Cognitive Behavioral Therapy (CBT) helps patients manage symptoms by changing their thoughts and behaviors, addressing the psychological aspects of chronic pain. Support groups provide emotional support and practical advice, offering a sense of community and shared experience. Stress management techniques like mindfulness, meditation, and relaxation exercises can reduce symptom severity. Maintaining a healthy lifestyle through diet and exercise improves overall well-being, while avoiding triggers such as caffeine or alcohol and ensuring adequate sleep can significantly impact symptom management. Integrating these lifestyle changes leads to a holistic improvement in health and a reduction in the severity and frequency of neurological symptoms. Medications such as pain relievers, antidepressants, and anticonvulsants can help manage symptoms. Pain relievers reduce discomfort, antidepressants address mood disorders and chronic pain, and anticonvulsants manage nerve pain and seizures. Physical therapy improves strength, coordination, and balance through tailored exercise programs and manual therapy techniques like massage. Cognitive Behavioral Therapy (CBT) helps patients manage symptoms by changing their thoughts and behaviors, addressing the psychological aspects of chronic pain. Support groups provide emotional support and practical advice, offering a sense of community and shared experience. Stress management techniques like mindfulness, meditation, and relaxation exercises can reduce symptom severity. Maintaining a healthy lifestyle through diet and exercise improves overall well-being, while avoiding triggers such as caffeine or alcohol and ensuring adequate sleep can significantly impact symptom management. Integrating these lifestyle changes leads to a holistic improvement in health and a reduction in the severity and frequency of neurological symptoms. Neurological Factors Neurological dysfunctions play a significant role in unexplained chronic pain. Nerve dysfunction, where the nervous system abnormally processes pain, and central sensitization, where the central nervous system becomes highly sensitive, are key factors. These conditions amplify pain responses even in the absence of an ongoing injury or disease. Psychological Factors Stress and anxiety can exacerbate pain perception. Chronic stress can lead to muscle tension and pain, while anxiety can heighten the body’s pain response. Depression is another critical factor, as it can both result from and contribute to chronic pain. The interplay between chronic pain and depression often creates a vicious cycle that is
Staying Fit for Family Fun in Nature: How Chiropractic Littleton CO can Help Parents
Staying Fit for Family Fun in Nature: How Chiropractic Littleton CO can Help Parents Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief Chiropractic Care in Littleton CO: Helping Parents Stay Active Living in Littleton, Colorado, offers families the best of both worlds—a family-friendly suburb with proximity to outdoor adventures. Whether you’re enjoying a day in South Platte Park or exploring the trails at Carson Nature Center, outdoor activities are a huge part of life here. For parents who want to keep up with their kids and explore Colorado’s great outdoors, staying physically fit is essential. Chiropractic care plays a significant role in helping parents maintain the strength and flexibility needed to keep up with Littleton’s active lifestyle. In this blog, we’ll explore how chiropractic care can help parents stay in peak shape, prevent injuries, and keep the whole family active and enjoying the beauty of nature. Keeping Up with Your Kids: The Challenge of Family Adventures Parenting is a full-body workout. Whether you’re pushing strollers, chasing after toddlers, or carrying gear for a family picnic, it’s no wonder many parents experience strain on their backs, necks, and joints. These physical demands can intensify when you’re navigating uneven terrain on hiking trails or spending long hours outdoors. The strain on your muscles and joints often leads to soreness or even injuries, making it harder to enjoy family activities. Chiropractic care can be a game-changer for parents, helping you stay fit, mobile, and injury-free. Regular adjustments realign the spine and reduce stress on muscles and joints, allowing your body to move more fluidly and handle the physical demands of parenting. Chiropractic care also helps to release tension built up from constant lifting, carrying, and bending over, keeping your body balanced. Keeping your body in optimal condition means more time exploring the outdoors with your family and less time dealing with aches and pains. At Denver Upper Cervical, we have all of the chiropractic specialties including rehabilitation, treatment for headaches, TMJ, post concussion syndrome and even vertigo! The Strain of Outdoor Adventures: How Chiropractic Can Help Littleton’s proximity to nature provides endless opportunities for hiking, biking, and camping. But the physical strain from these activities can take a toll on your body, especially if you’re not used to the challenges of rugged terrain. Hiking, in particular, puts strain on the knees, ankles, and lower back. Walking uphill can cause stress on the muscles and joints, and downhill hikes can increase pressure on your knees. Activities like hiking can exacerbate knee pain caused by overuse, improper footwear, or carrying heavy loads. Mountain biking, a popular outdoor activity in Colorado, is also associated with wrist fractures and shoulder dislocations from falls and impacts. Symptoms of wrist fractures include pain, swelling, and difficulty moving the wrist. When it comes to biking, poor posture and improper gear can also contribute to joint pain. Chiropractic care can help manage these injuries by promoting proper alignment, reducing pain, and speeding up recovery. Through regular chiropractic adjustments at Denver Upper Cervical, you can minimize the risk of repetitive strain injuries and keep your body in top condition. Shoulder dislocations, which often occur from falls while biking, require immediate care and rehabilitation. Chiropractic adjustments, combined with physical therapy, can help strengthen the shoulder and prevent future dislocations. Regular chiropractic care will help parents enjoy biking and other outdoor activities without the fear of recurring injuries. Preventing Common Injuries: Stay Active with Your Kids Outdoor adventures in Littleton are exciting, but they also come with risks of injury. Whether you’re hiking, playing sports with your kids, or biking on rugged trails, you’re bound to face physical challenges. Other common injuries, such as ankle sprains and knee pain, can easily occur when navigating uneven terrain during hikes or other outdoor activities with your kids. Ankle sprains are a common injury caused by overstretching or tearing the ligaments, often from stepping on uneven surfaces or sudden twisting motions. In active families, falls from mountain bikes or while hiking can also lead to wrist fractures and shoulder dislocations, especially if proper care is not taken. Chiropractic care is key to not only treating these injuries but also preventing them through improved joint stability and flexibility. By addressing the root causes of musculoskeletal problems, chiropractic care ensures that your body can recover quickly from minor injuries and remain resilient during physical activities. Regular chiropractic care can also promote better posture and alignment, which can reduce the risk of overuse injuries. Strengthening exercises recommended by our chiropractor at Denver Upper Cervical will also help reinforce weak joints and support long-term health. For parents who want to enjoy activities like mountain biking without injury, regular chiropractic care is essential for keeping joints and muscles in optimal condition. Family Wellness: A Holistic Approach to Outdoor Adventures At Denver Upper Cervical, we believe in a holistic approach to family wellness. This means focusing on your entire body’s health, from improving mobility to reducing stress and tension. Chiropractic care is more than just adjustments; it’s about supporting your overall health and well-being so that you can enjoy a full and active life with your family. By addressing misalignments in the spine and nervous system, chiropractic care enhances your body’s natural ability to heal, helping you remain active and energetic. Research shows that chiropractic care can support overall health by improving the nervous system’s function, enhancing your body’s ability to adapt to the physical demands of outdoor adventures. Our gentle, NUCCA-based chiropractic adjustments are designed to align the upper cervical spine, ensuring that your body can function at its best. We take a personalized approach, making sure that our care is tailored to the specific needs of each patient, helping you maintain long-term health and performance. With our focus on precise, gentle care, we help you maintain flexibility and strength while reducing pain and discomfort, allowing you to keep up with your kids in nature. What to Expect at Denver Upper Cervical When you visit Denver Upper Cervical, you can expect a personalized approach to your care. Your first appointment
Headaches: Causes, Treatments, & Types
Headaches: Causes, Treatments, & Types Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief Did you know that your average headache relief medication is simply hiding the symptoms of your headache? Imagine if proper treatment was to address the root cause of headaches . 45 million Americans suffer from chronic headaches each year. Up to 4% of the world’s population experience chronic daily headaches. There are many different types of headaches, such as migraines or tension headaches. Some types stem from different root causes. At Denver Upper Cervical Chiropractic, we believe in treating the underlying causes of headaches. A headache is your body’s way of telling you something is wrong — and you can often fix what’s truly wrong with the right care. Even some traditional medicines are just masking the symptoms of your headaches, instead of treating the underlying cause. In other words, you may not have a headache because you are ginger-deficient. Let’s take a look at what a headache is, what causes them, and how to treat the root causes. What causes a headache? A headache (AKA head pain) is caused by many different headache triggers. For instance, a primary headache is likely caused by abnormal activity around structures in the head that are pain-sensitive. This can involve muscular activity, blood vessels, and nerves in the head or neck. A tension headache can be caused by stress and bad posture. Another common cause is strenuous activity. However, a secondary headache has all sorts of potential root causes. You can get a secondary headache due to dehydration, medication overuse, caffeine withdrawal, allergies, infections, or issues with your spine. It is important that you consult a healthcare professional to help identify the root cause of your headache. It may be a simple fix, such as diet, stress relief, or a chiropractic adjustment. If you live in the greater Denver area, click here to request an appointment at Denver Upper Cervical Chiropractic. We reserve Fridays for out-of-town patients. Types of Headaches Primary Headaches Primary headaches are thought to be triggered by issues in your blood vessels — often benign issues that only lead to headaches, nothing else. Primary headache disorders make up more than 90% of headache-related pain. There are four main types of primary headache: tension, migraine, cluster headaches, and hemicrania continua. Tension Headaches Migraines Cluster Headaches Hemicrania Continua First on our list, tension headaches are the result of bad posture or stress. This causes the back of the neck and your scalp muscles to tighten. A tension headache feels like the sides of the head are squeezing in. A tension-type headache is the most common type of headache. Women over 20 years old are at highest risk. Noise and stuffy environments can strengthen a tension headache. Tension headaches can last for minutes or days. Secondary Headaches Secondary headaches are caused by an underlying medical condition instead of just an abnormality in your blood vessels. These are less common, but still important to understand. Since it is important to treat the root cause of your headache — not just mask the symptoms — it can be helpful to see all the possible secondary causes laid out for you. Here are the twelve common types of headaches (secondary) you need to understand : Migraine headaches are the second most common kind of headache. Chronic migraines affect millions of Americans every year. Many consider this the worst headache you can get. Migraine symptoms include intense throbbing pain, stiff neck, and anxiety. It can be accompanied by light or noise sensitivity. Where tension headaches cause tension on both sides of your head, a migraine is usually on only one side of your head. Migraines can last hours, or even days. Some people will experience an “aura” (a set of visual symptoms) before a migraine attack: Bright spots Flashing lights Moving lines Temporary loss of vision (in severe cases) The third most common primary headache is the cluster headache, which affects about a million people in the United States each year. A cluster headache does not throb. They are often felt behind an eye or on one side of the head only. Cluster headaches can occur multiple times a day, and they are more common in adult men. A cluster headache is likely triggered by increased blood flow due to widening blood vessels. This is a rare headache disorder. Hemicrania continua exhibits headache symptoms but usually only on one side of the head. The cause is unknown, but hemicrania continua persists, with only a handful of documented remissions. First on our list, tension headaches are the result of bad posture or stress. This causes the back of the neck and your scalp muscles to tighten. A tension headache feels like the sides of the head are squeezing in. A tension-type headache is the most common type of headache. Women over 20 years old are at highest risk. Noise and stuffy environments can strengthen a tension headache. Tension headaches can last for minutes or days. Secondary Headaches Secondary headaches are caused by an underlying medical condition instead of just an abnormality in your blood vessels. These are less common, but still important to understand. Since it is important to treat the root cause of your headache — not just mask the symptoms — it can be helpful to see all the possible secondary causes laid out for you. Here are the twelve common types of headaches (secondary) you need to understand : Migraine headaches are the second most common kind of headache. Chronic migraines affect millions of Americans every year. Many consider this the worst headache you can get. Migraine symptoms include intense throbbing pain, stiff neck, and anxiety. It can be accompanied by light or noise sensitivity. Where tension headaches cause tension on both sides of your head, a migraine is usually on only one side of your head. Migraines can last hours, or even days. Some people will experience an “aura” (a set of visual symptoms) before a migraine attack: Bright spots Flashing lights Moving lines Temporary loss of vision (in severe cases) The third most common primary headache is
Migraine vs. Headache: Differences & Treatments
Migraine vs. Headache: Differences & Treatments Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief Have you ever asked someone if they have a headache, and they said, “No, it’s a migraine”? You both are correct. A migraine is a specific type of headache. Migraine headaches have unique migraine symptoms though. They’re also a leading cause of workplace disability. Migraines and other types of headache pain require unique treatments, too Below, I’ll discuss the differences between migraines and all other headache types — and how to effectively treat both. Headaches: Types & Causes There are several types of headaches other than migraine headaches. Let me briefly run through the most important types. Tension headaches are the most common headache type. Symptoms include tightening in the back of the neck and scalp, as well as pain on both sides of the head. Stress and bad posture are generally the triggers of tension-type headaches. Cluster headaches are the third most common headache type. Cluster headaches are not throbbing. They can be felt behind the eye or on one side of the head. These are thought to be caused by increased blood flow from widening blood vessels. Cervicogenic headaches are brought on by bad posture, a pinched nerve, osteoarthritis, whiplash injury, or prolapsed disc. They can mimic symptoms of migraines, and are most effectively treated with upper cervical chiropractic care. Medication overuse headaches , formerly known as rebound headaches, happen when you decrease the dosage or altogether stop taking a medicine that you were taking too much of in the first place, such as acetaminophen. Sinus headaches occur when your sinuses are inflamed, typically due to the medical condition sinusitis. This triggers unusual pressure which causes a headache. There are more types of headaches less common than the ones I just mentioned, such as sugar headaches and caffeine headaches. Read in depth about all the headache types here . Migraine: Symptoms & Triggers Migraine sufferers often claim their migraine pain is worse than a normal headache. They’re right; the symptoms can be worse. How do you know you have a migraine? The symptoms of migraine headaches can be easy to spot, whether people experience a mild or severe migraine attack: Intense, throbbing pain on only one side of the head Nausea, upset stomach Light, noise, and smell sensitivity bnormal body temperature Dizziness Unfortunately, there are also prodrome symptoms, which means symptoms that occur in the day or two leading up to a migraine attack: Anxiety, irritability Stiff neck Constant yawning Constipation What is migraine with aura? Migraine headaches can present with or without aura, which is a set of visual disturbances. Symptoms of aura may appear thirty minutes before migraine head pain starts. They include: Bright spots Flashing lights Moving lines Hearing sounds that aren’t there In severe cases, temporary loss of vision What can trigger migraines? Common migraine triggers include: Stress Certain foods Fasting Physical activity Lack of sleep, change in sleep pattern Smoking Excess alcohol Certain smells Changes in weather Menstruation or other hormonal changes How can you tell the difference between a headache & migraine? The differences between migraines and other headaches can be subtle. Sometimes, it’s more obvious. Migraines are typically more painful and debilitating. Migraine headaches usually last for between four and 72 hours, whereas tension headaches last between 30 minutes and one week, if left untreated. The most common headache — tension headache — triggers pressure around both your temples and forehead. But if the pain is beyond moderate, it’s probably a migraine. Can a headache turn into a migraine? For an unfortunate few, tension headaches can trigger migraines. This is likely due to the stress of a headache causing a migraine to develop. Although we always encourage patients to treat underlying causes of headaches, taking a pain reliever can stop the tension headache before it leads to a more painful migraine. Effective Treatments for Headache + Migraine We compiled a list of easy treatment options for getting rid of your headache symptoms or chronic migraines. It’s wise to discuss some of these lifestyle changes with your doctor or neurologist. Chiropractic care is a common and effective treatment for headaches and can relieve migraine pain. There’s a reason we at Denver Upper Cervical Chiropractic believe in the power of spinal alignment — we’ve seen it work hundreds of times. If you live in the greater Denver area, click here to request an appointment with us. We reserve Fridays for out-of-town patients. A healthy diet is key to preventing migraines. Avoid food additives. If you are prone to headaches, try cutting out potential migraine triggers like wheat and dairy. Supplementing riboflavin (vitamin B2) or magnesium has shown promise in preventing migraines. Good hydration may prevent headaches as well. A regular sleep schedule is key. Not only does a good night’s sleep reduce stress , a sleep routine can decrease potential migraine triggers. Excessive caffeine consumption may lead to headaches. But caffeine withdrawal is a more common cause of headaches. Relaxation techniques can reduce stress: meditation , yoga, going outside. Stress is a trigger for both tension headaches and migraines. If you’re looking for temporary pain relief, there are a few options — both over-the-counter medicines and all-natural remedies. Keep in mind, the pharmaceuticals in this list come with some potentially nasty side effects, particularly when used in excess. Curcumin Ginger Peppermint oil Lavender oil Aspirin Acetaminophen Sumatriptan Blood pressure medication NSAIDs (non-steroidal anti-inflammatory drugs), like ibuprofen and naproxen In Summary Migraines can be debilitating. Usually on just one side of the head, migraine attacks can result in nausea or dizziness. An aura (visual symptoms) can occur thirty minutes or so before a migraine. Symptoms of migraine with aura include seeing moving lines and bright lights. The most common type of headache is tension headache, caused by stress or bad posture. This usually occurs on both sides of the head. What is the difference between a headache and a migraine? Simply put, migraines are worse — a leading cause of workplace disability. If you have sudden and severe headaches, especially after a head injury, seek medical attention immediately. Also, if a headache causes vomiting, vision loss, difficulty speaking or moving, or partial paralysis, get to a doctor right away.
Basilar Migraine: Triggers, Symptoms, Treatment & Prevention
Basilar Migraine: Triggers, Symptoms, Treatment & Prevention Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief Millions of Americans suffer from migraines every year, but one specific type of migraine comes with some trippy visual symptoms. Basilar migraines are a strange phenomenon, not well understood in the conventional medical community. These migraines start in the brain stem and are preceded by an “aura,” which is a set of visual symptoms, like seeing flashing lights that are not actually there. It can be important to recognize the symptoms of a basilar migraine as well as discuss the potential causes of this medical condition. The pharmaceutical industry thrives on masking symptoms but leaving root causes untouched. That way, the underlying cause keeps causing problems, and you have to continue buying medication. At Denver Upper Cervical Care, our patients actually get better. Each person’s body has the ability to heal — if we simply address the root cause. Basilar migraines are a bit mysterious, but there are several known risk factors that you can reduce. You can also learn about the 16 best treatment options if you read below. What are basilar migraines? Are they dangerous? Basilar migraines are a migraine type that lasts about an hour and begins in your brain stem. Scientists are not 100% sure what exactly the cause is. Many believe basilar migraines occur due to vasoconstriction, or the narrowing of blood vessels. The muscular wall of the vessel tightens and constricts blood flow. These types of migraines are sometimes called basilar artery migraines because some believe that a spasm of the basilar artery might be the main culprit behind these migraine attacks. Actually, this is a less and less common theory, and “basilar migraine” is no longer the recommended term. What is a migraine with brainstem aura? Are basilar migraines dangerous? Migraine with brainstem aura is the most recent term recommended for use by the International Headache Society (IHS). However, both “basilar migraine” and “migraine with brainstem aura” can still be used interchangeably at this point. An aura can be scary the first time you experience it. A typical aura occurs less than an hour before the head pain starts. A migraine aura is a set of visual symptoms that can accompany a migraine. All basilar migraines come with aura symptoms. Basilar migraines are sometimes called Bickerstaff migraines, named after Edwin R. Bickerstaff who first identified the condition in 1961. This relatively rare type of migraine headache can be dangerous. Basilar migraines seem to increase your risk of ischemic stroke, especially in women who take contraceptives. Also, basilar migraines can decrease your level of consciousness or awareness. This means you don’t want to get a basilar migraine while you’re driving. Migraine with brainstem aura is the most recent term recommended for use by the International Headache Society (IHS). However, both “basilar migraine” and “migraine with brainstem aura” can still be used interchangeably at this point. An aura can be scary the first time you experience it. A typical aura occurs less than an hour before the head pain starts. A migraine aura is a set of visual symptoms that can accompany a migraine. All basilar migraines come with aura symptoms. Basilar migraines are sometimes called Bickerstaff migraines, named after Edwin R. Bickerstaff who first identified the condition in 1961. This relatively rare type of migraine headache can be dangerous. Basilar migraines seem to increase your risk of ischemic stroke, especially in women who take contraceptives. Also, basilar migraines can decrease your level of consciousness or awareness. This means you don’t want to get a basilar migraine while you’re driving. Symptoms of a Basilar Migraine Although basilar migraines feature aura symptoms, which can be a little frightening, these symptoms of migraines with brainstem aura include more than just visual symptoms. Headache pain on one or both sides of your head Vertigo Lack of coordination Confusion Slurred speech Nausea Double vision Temporary loss of hearing, ringing in your ears Loss of muscle control Loss of consciousness Aura symptoms (last for about 20 minutes, occur before migraine): Seeing flashing lights Seeing spots, lines Seeing static Weakness, exhaustion Numbness in head, hands, or face Temporary vision loss Diagnosis There are several medical conditions easily confused with basilar migraines. A clinical diagnosis is very important to distinguish between a basilar-type migraine and a brain disorder. The International Classification of Headache Disorders (ICHD) 3rd edition provides us with detailed diagnostic criteria : At least two migraine attacks (which fulfill 2 and 3 below) Aura, consisting of temporary visual/sensory/speech symptoms, but no motor or retinal symptoms At least two of the following symptoms: Slurred speech (dysarthria) Double vision (diplopia) Temporary loss of hearing (hypacusis) Ringing in your ears (tinnitus) Loss of muscle control (ataxia) Numbness on both sides of your body (bilateral paresthesia) Vertigo Decreased level of consciousness At least two of the following characteristics: At least one aura symptom over the course of five minutes Two or more aura symptoms occur in succession Aura symptoms last 5-60 minutes At least one aura symptom is unilateral The aura is followed by headache pain Transient ischemic stroke and other similar diagnoses have been ruled out To rule out neurological diseases, you may need to see a neurologist. The neurologist may administer a magnetic resonance imaging (MRI) scan or computer tomography (CT) scan to rule out a number of brain disorders, or an electroencephalogram (EEG) to rule out seizures. What conditions might your doctor want to rule out before treating you for migraines with brainstem aura? Stroke Epilepsy Meningitis Vestibular disorder Vertebrobasilar disease Meniere’s disease Brainstem arteriovenous malformation Brain tumor Basilar migraines are similar in nature to familial hemiplegic migraines. Hemiplegic migraines uniquely include weakness on one side of your body, as well as trouble speaking. A clear diagnosis will distinguish between the two. Causes & Risk Factors Scientists do not know exactly why basilar migraines occur. But there are certain risk factors that have been attributed to basilar migraine attacks: Stress (physical or emotional) Lack of sleep (or, in rarer cases, excessive sleep) Poor posture Motion sickness Alcohol Caffeine Dietary nitrites (like in hot dogs) Being overweight,
What Causes Body Aches? Remedies & Red Flags
What Causes Body Aches? Remedies & Red Flags Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief Whether we sit around all day, or we work our fingers to the bone, our bodies ache. Especially when a global pandemic forces most of us to spend hours and hours sitting around the house, it is important to understand how body aches are triggered and how to remedy them. Body aches are when parts of your body experience a continuous dull pain. Though body aches vary in intensity and frequency , they are very common. But just because they are common doesn’t mean you have to live with them. Aching can be caused by several various factors, such as tiredness, stress, a cold, or even a vitamin deficiency. Below, you will learn about remedies for body aches, as well as when you should seek help. Causes of Body Aches So many factors can cause your body to ache. You might ask, “Does lack of activity make my body ache?” Yes, sitting for a long time, working for a long time, the flu — a lot of triggers can make your body ache: Sitting, or standing in the same position for a long period of time Poor posture Prolonged physical labor Chronic fatigue syndrome Lack of sleep Stress Dehydration Flu (influenza) Common cold Pneumonia Mononucleosis (also called “mono” or “the kissing disease”) Other bacterial and viral infections Lyme disease (infection from a tick bite) Fluid retention (which can be caused by congestive heart failure, hypothyroidism, etc.) Vitamin D deficiency (AKA hypocalcemia) Arthritis Anemia Hypokalemia Fibromyalgia Lupus Multiple sclerosis (also known as MS) Myositis Withdrawal from drugs or alcohol Certain medications (for example, blood pressure meds or statins) Read Next: Can Chiropractic Care Treat Trigeminal Neuralgia? Remedies for Ongoing Body Aches There are ways to alleviate the common symptoms of body aches, and there are ways to address the underlying causes. Although we suggest addressing these root causes , you may also want immediate relief from muscle aches and joint pain. Rest & Relaxation Fight Dehydration Chiropractic Care Over-the-Counter Medications All Natural Pain Relievers Rest & Relaxation Rest is a wonderful thing. Your body needs time to repair and recuperate. Putting your legs up and unwinding from a stressful day can prevent or alleviate body aches. Sleep can take it a step further. Getting a full night’s sleep (seven to eight hours a night) has been linked to less pain throughout the body. If you’re having trouble sleeping, try taking a warm shower or drinking hot tea an hour before bedtime. Cutting out blue light emissions is one way to get high-quality sleep. Technology like your phone and television emit blue light, which tricks your brain into thinking the sun is still up. Turn off technology an hour before bedtime, so your mind can naturally want to fall asleep. Stress relief should reduce your anxiety and reduce your risk for body aches — not to mention a lot of other medical conditions. Prolonged stress weakens your immune system and has been linked to a lot of nasty diseases. Relaxation techniques include: Meditation Yoga Acupuncture Massage Having a warm bath Enjoying the outdoors Spending less time on social media Share your feelings of stress with someone you trust, like a friend or therapist Fight Dehydration Drink plenty of fluids . Dehydration can cause headaches and muscle weakness. Prevent these aches by staying hydrated. Other symptoms of dehydration to look out for include: Dark urine Exhaustion Disorientation Dry mouth or tongue Extreme thirst Chiropractic Care Chiropractic care can help you when you’re feeling achy. Chiropractic adjustments have been shown to reduce neck pain and low back pain. Regular visits ensure that your skeletal base is providing balanced support to each segment of your body. Not only does chiropractic manipulation help cure acute and chronic pain, it has been shown to alleviate headaches and boost your immune system’s communication. If you live in the greater Denver area, click here to request an appointment at Denver Upper Cervical Chiropractic. For your convenience, we reserve Fridays for out-of-town patients. Over-the-Counter Medications Non-steroidal anti-inflammatory drugs (NSAIDs), like ibuprofen or naproxen or aspirin, are known to reduce pain and inflammation. They treat the symptoms and not the causes, but can be an effective way to relieve short-term pain. However, many avoid overuse of NSAIDs due to their side effects. Acetaminophen (Tylenol) is another over-the-counter medication you can take for pain relief. For some, acetaminophen is a great way to reduce flu symptoms. All Natural Pain Relievers Ginger is well-known for its ability to reduce swelling, inflammation, and general pain. This makes it the perfect all-natural pain reliever that you can find in a dietary supplement or on your spice rack. Curcumin is the primary component in turmeric. Curcumin has been shown to reduce aches and pains. Studies show that curcumin is antioxidant, antimicrobial, anti-inflammatory, and even anti-cancer. Though the bioavailability of curcumin from the spice turmeric is low, you can find curcumin in dietary supplement form. Lavender is a known natural pain reliever. Lavender oil and lavender aromatherapy are both research-backed methods of getting rid of body aches. Rosemary essential oil is a common analgesic, which means it relieves pain. Rosemary essential oil can help you say goodbye to body aches. Peppermint is a commonly used pain therapy. Whether via essential oil or via aromatherapy, peppermint has been used to alleviate abdominal pain, shoulder pain, and general aching. Cloves are another popular all-natural pain reliever. Clove oil contains eugenol, which is an anti-inflammatory agent. A lot of pain comes from inflammation, so reducing inflammation can lead to less body aches. Feverfew is the name given to a flower by the scientific name Tanacetum parthenium. It “behaves as a potent pain reliever ” in all sorts of cases. Inflammatory pain, neuropathic pain, acute pain — feverfew seems to relieve all kinds of aching. Always consult your healthcare provider before starting any new dietary supplement. Some may interact poorly with synthetic drugs you may be taking. When It’s Time to Call Your Doctor “How do I know when a body ache is serious?” You know when a body ache is serious when it is accompanied by warning signs that indicate a dangerous root cause.