Headache on Top of Your Head? Here’s Why and How to Fix It
Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief
If you’ve ever experienced head pain, you understand the urgent need for relief. Specifically, a headache on top of the head may be treated long-term with improved sleep, sleep apnea treatment, limiting caffeine, or other treatments that address potential root causes.
What are the symptoms of a headache on top of the head?
- Constant or throbbing pain on top of head
- Tightening sensation
- Pressure
- Neck pain
- Jaw pain
- Sensitivity to light or noise
- Throbbing pain or pressure in the crown
Good news: Headaches on the top of the head are rarely life-threatening, but they can still be disruptive and painful. Keep reading to learn more about the common causes of these headaches and how you can keep them from happening.
1. Sleep Problems
2. Dehydration
3. Tension Headaches (Poor Posture)
4. Medication Side Effects
5. Inconsistent Caffeine Consumption
6. Head Injury
7. Teeth Grinding (Bruxism)
8. Sinus Problems
9. Migraines
10. Occipital Neuralgia
Inconsistent and low-quality sleep are common causes of headaches, including top-of-head headaches.
In fact, one of the major symptoms of many sleep disorders is getting frequent headaches. Going to sleep or taking a nap may stop some headaches.
Dehydration may lower brain fluid levels, causing the brain to shrink slightly and pull away from the skull. This shrinking places excess pressure on nerves and causes pain on the top of your skull.
Drinking too much alcohol may lead to dehydration — since alcohol is a diuretic that flushes fluids through your renal system.

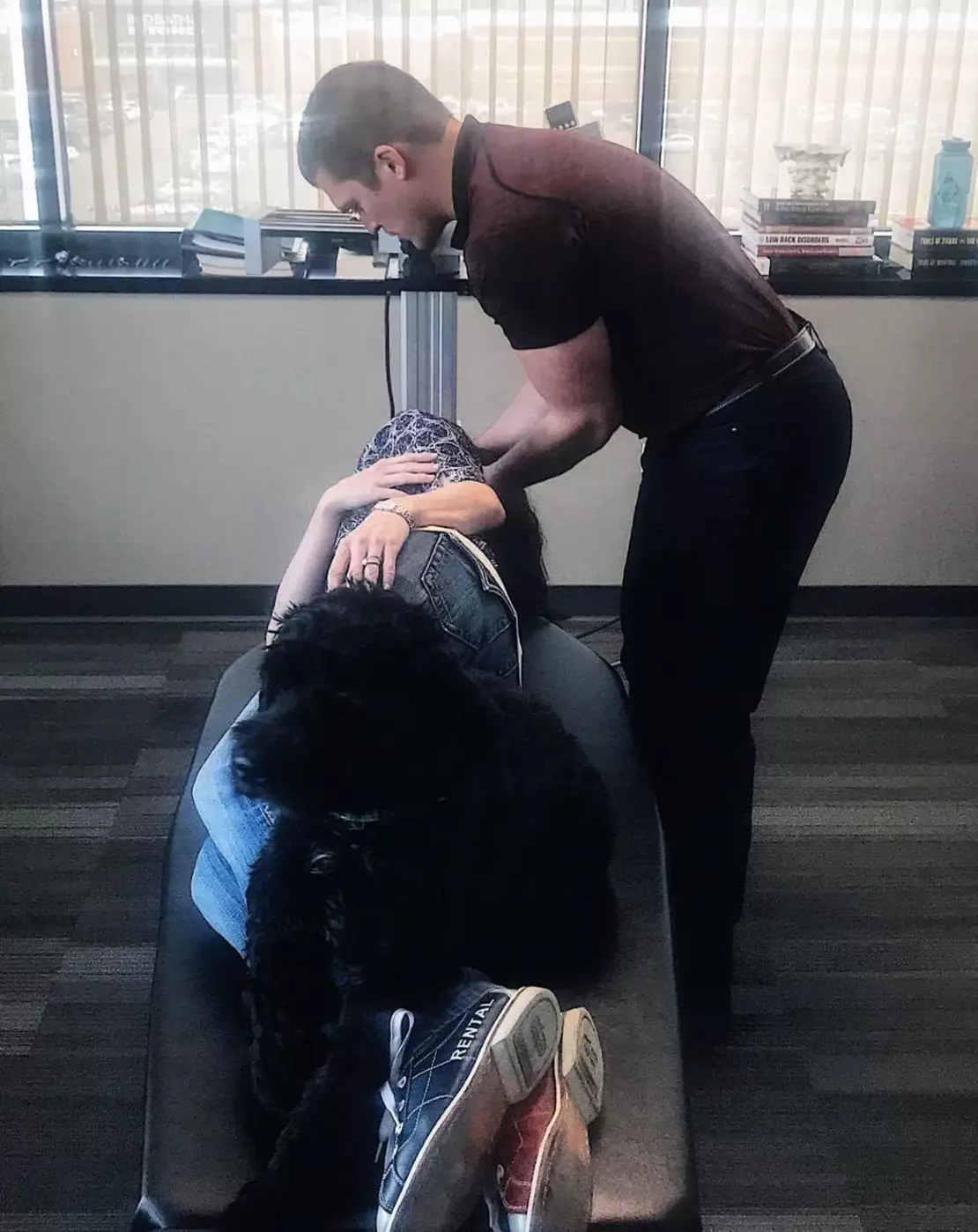
Tension-type headaches might be causing your top-of-head headaches, especially if you sit in front of a computer all day.
Holding your head too far forward puts stress on the muscles and bones at the top of your neck, which leads to headaches all over your head: on top, on the sides, and in the back of the head.
What is a tension headache ? Tension headaches are the most common type of headache. They can happen for many reasons, including poor posture, muscle overuse, and spinal misalignment, which results in muscle tension that travels up to the top and sides of your head.
Many medications have headache pain as a side effect.
Even if headache isn’t listed as a side effect, overusing over-the-counter or prescription pain reliever medications can lead to rebound headache or medication overuse headache.
These headaches that may occur on the top of your head typically occur when patients frequently use medications to treat their recurrent headaches over a long period.
Caffeine consumption can lead to rebound headaches, particularly if you’re used to drinking caffeine every day, or you’re trying to reduce how much caffeine you drink.
Having too much or too little caffeine is a common culprit of head pressure on top of the head
Head trauma can lead to chronic headaches on top of the head, regardless of how severe the head injury was or how long ago it happened.
Research actually suggests that minor head injuries may be more likely to cause chronic daily headaches , cluster headaches, and other adverse symptoms.


A major cause of headache disorders (particularly morning headaches ) is grinding the teeth, also called bruxism.
Many people with bruxism grind their teeth while asleep, impacting the muscles, bones, and joints of the jaw and skull and leading to top-of-head headaches in adults.
Sinuses are hollow cavities in the skull. Sinus headaches and sinus infections typically feel painful in the nasal area, cheeks, jaws, and teeth.
However, patients with a sinus headache may also feel sharp pain at the top of the head.
Migraines are severe headaches that feel like a throbbing pain usually on one side of the head, possibly the top of your head. Migraines can happen with or without auras — visual or auditory disturbances that often precede migraine pain.
Common migraine triggers include:
- Stress
- Too much light
- Certain smells
- Hormone changes
- Changes in the weather
- Diet, such as chocolate, dairy, or processed meat
Three major occipital nerves run up from the spinal cord toward the top of the head. These nerves can become inflamed, leading to occipital neuralgia — a headache often described as either a piercing or a throbbing pain.
What causes a headache on top of your head ? Occipital neuralgia, migraines, poor posture, head injuries, and certain medications all cause your head to hurt at the top of your head. There are rare, more severe possible causes, such as high blood pressure or a brain tumor.

Rare Causes of a Headache on Top of Your Head
Below are a few rarer causes of headache pain on top of your head:

Blood vessel constriction
Constricting blood vessels in the head and brain can also cause pain at the top of your head. In some cases, these headaches are caused by reversible cerebral vasoconstriction syndrome (RCVS), a rare syndrome sometimes referred to as thunderclap headaches .

Brain aneurysm
In the most severe case, a blood vessel may rupture in the brain, leading to severe headache. Other than a headache, symptoms of a brain aneurysm include generally feeling unwell, dizziness, confusion, seizures, unexplained muscle weakness, blurry vision, and a sensitivity to light. A cerebral aneurysm requires immediate medical attention.

Hypertension Headaches
Hypertension headaches happen when high blood pressure makes the pressure in and around your brain rise, which causes pain. These headaches can be a symptom of life-threatening high blood pressure, so seek medical care immediately if you have hypertension and a bad headache.

Hypnic Headaches
These are headaches associated with disordered sleep. Nighttime headaches on top of your head may be caused by hypnic headache pain.

Brain tumor
In rare cases, a tumor may cause severe pain on top of your skull. Talk to your healthcare provider about other symptoms of having a tumor.
Treatments
If you suffer from headaches at the top of your head, you don’t have to live with that pain. There are highly effective treatment options to help treat headache pain when it happens and to help stop headaches from developing in the first place.
Below are the most common ways to treat headaches on top of the head:
- Medication: Over-the-counter (OTC) pain relievers like acetaminophen, non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen, and muscle relaxants (prescription required) may treat different kinds of headaches. Antidepressants may also be prescribed, but the side effects often outweigh the benefits.
- Chiropractic adjustments : Adjustments from a qualified chiropractor often treat headaches , particularly headaches that keep recurring. Many headaches, including headaches on top of the head, are caused by poor posture, spinal misalignment , and neck position. Chiropractic care helps bring your spine into alignment.
- Acupuncture: Studies show that acupuncture is a significant pain reliever for headache sufferers.
- Massage: Especially if a headache is caused by muscle tension, massaging the affected muscles can reduce head pain.
- Anti-inflammatory supplements : Fish oil, ginger, butterbur, and vitamin D may help reduce inflammation that contributes to headaches. Vitamin B2 and magnesium may help with migraine headaches. These supplements are not recommended in the long term since they may not address your underlying health condition.
Here are the best ways to prevent top-of-head headaches:
- Keep caffeine consumption consistent: Consuming too much (or too little) caffeine is an easy way to get a headache. Keep your caffeine intake constant, and don’t quit caffeine cold turkey. Don’t drink caffeine fewer than 8 hours before you go to bed.
- Get enough sleep : Lack of sleep is a major headache trigger. Try to wake up at consistent times. Get 7-8 hours of quality sleep every night for your head (and for your overall health).
- Reduce stress: Chronic stress contributes to many medical conditions, including headaches. Relaxation techniques such as yoga, meditation, prayer, or spending time outside may work for you. Consider stress-relieving lifestyle changes such as regular exercise.
- Reduce alcohol intake: Drinking too much alcohol can cause dehydration headaches, and not just when you’re hungover. If you tend to get headaches after drinking, consider reducing or eliminating alcohol intake.
- Practice good posture: If poor posture is causing tension headaches on top of your head, change your posture. Practice ideal posture while sitting, working, driving, sleeping, etc.
How do you get rid of a headache on the top of your head naturally? You get rid of a headache on the top of your head immediately by taking medication. Still, all-natural chiropractic treatment may naturally correct the root cause of the headache for a more permanent solution. Healthy sleep, massage, or stress relief may also relieve a headache.
When To Seek Headache Help in Denver, CO
If you have an excruciatingly painful headache, head to the emergency room for medical advice. In the long term, seek out a chiropractor to identify if spinal misalignment is the underlying cause of the headache on top of your head.
You should seek immediate medical attention if any of the following severe symptoms accompany a sudden headache:
- Stiff neck
- Dizziness, vertigo
- Nausea, vomiting
- Losing consciousness
- Losing vision in one or both eyes
- Headache pain right after recent head injury
Schedule an appointment with Denver Upper Cervical Chiropractic, and together, we’ll address your unique headache triggers through a personalized treatment plan . I look forward to working with you and helping you say goodbye to chronic headaches.
Sources:
- Korabelnikova, E. A., Danilov, A. B., Danilov, A. B., Vorobyeva, Y. D., Latysheva, N. V., & Artemenko, A. R. (2020). Sleep disorders and headache: A review of correlation and mutual influence. Pain and therapy , 9 (2), 411-425. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7648824/
- Elizagaray-Garcia, I., Beltran-Alacreu, H., Angulo-Díaz, S., Garrigos-Pedron, M., & Gil-Martinez, A. (2020). Chronic primary headache subjects have greater forward head posture than asymptomatic and episodic primary headache sufferers: Systematic review and meta-analysis. Pain medicine , 21 (10), 2465-2480. Full text: https://www.researchgate.net/profile/Ignacio-Elizagaray-Garcia-2/publication/345144818_Chronic_Primary_Headache_Subjects_Have_Greater_Forward_Head_Posture_than_Asymptomatic_and_Episodic_Primary_Headache_Sufferers_Systematic_Review_and_Meta-analysis/links/61c44cd7c99c4b37eb1878af/Chronic-Primary-Headache-Subjects-Have-Greater-Forward-Head-Posture-than-Asymptomatic-and-Episodic-Primary-Headache-Sufferers-Systematic-Review-and-Meta-analysis.pdf
- Fischer, M. A., & Jan, A. (2019). Medication-overuse headache. Full text: https://www.ncbi.nlm.nih.gov/books/NBK538150/
- Jovel, C. E., & Mejía, F. S. (2017). Caffeine and headache: specific remarks. Neurología (English Edition) , 32 (6), 394-398. Full text: https://www.sciencedirect.com/science/article/pii/S2173580817300858
- Leung, A. (2020). Addressing chronic persistent headaches after MTBI as a neuropathic pain state. The Journal of Headache and Pain , 21 (1), 77. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7304149/
- Kaur, A., & Singh, A. (2013). Clinical study of headache in relation to sinusitis and its management. Journal of Medicine and Life , 6 (4), 389. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3973877/
- Kikkeri, N. S., & Nagalli, S. (2022). Migraine with aura. In StatPearls [Internet]. StatPearls Publishing. Full text: https://www.ncbi.nlm.nih.gov/books/NBK554611/
- Ruschel, M. A. P., & De Jesus, O. (2023). Migraine headache. In StatPearls [Internet]. StatPearls Publishing. Full text: https://www.ncbi.nlm.nih.gov/books/NBK560787/
- Al Khalili, Y., & Chopra, P. (2020). Hypnic Headache. Full text: https://www.ncbi.nlm.nih.gov/books/NBK557598/
- Arca, K. N., & Halker Singh, R. B. (2019). The hypertensive headache: a review. Current pain and headache reports , 23 , 1-8. Full text: https://www.iranheadache.ir/wp-content/uploads/2020/04/The-Hypertensive-Headache-a-Review.pdf
- Jersey, A. M., & Foster, D. M. (2018). Cerebral aneurysm. Full text: https://www.ncbi.nlm.nih.gov/books/NBK507902/
- Vernon, H., Borody, C., Harris, G., Muir, B., Goldin, J., & Dinulos, M. (2015). A randomized pragmatic clinical trial of chiropractic care for headaches with and without a self-acupressure pillow. Journal of manipulative and physiological therapeutics , 38 (9), 637-643. Abstract: https://pubmed.ncbi.nlm.nih.gov/26548737/
- Al Khalili, Y., Ly, N., & Murphy, P. B. (2018). Cervicogenic headache. Full text: https://www.ncbi.nlm.nih.gov/books/NBK507862/
- Urits, I., Patel, M., Putz, M. E., Monteferrante, N. R., Nguyen, D., An, D., … & Viswanath, O. (2020). Acupuncture and its role in the treatment of migraine headaches. Neurology and therapy , 9 , 375-394. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7606388/
- Jimenez, M. P., DeVille, N. V., Elliott, E. G., Schiff, J. E., Wilt, G. E., Hart, J. E., & James, P. (2021). Associations between nature exposure and health: a review of the evidence. International Journal of Environmental Research and Public Health , 18 (9), 4790. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8125471/
The post Headache on Top of Your Head? Here’s Why and How to Fix It appeared first on Denver Upper Cervical Chiropractic.
© 2026 Denver Upper Cervical Chiropractic

