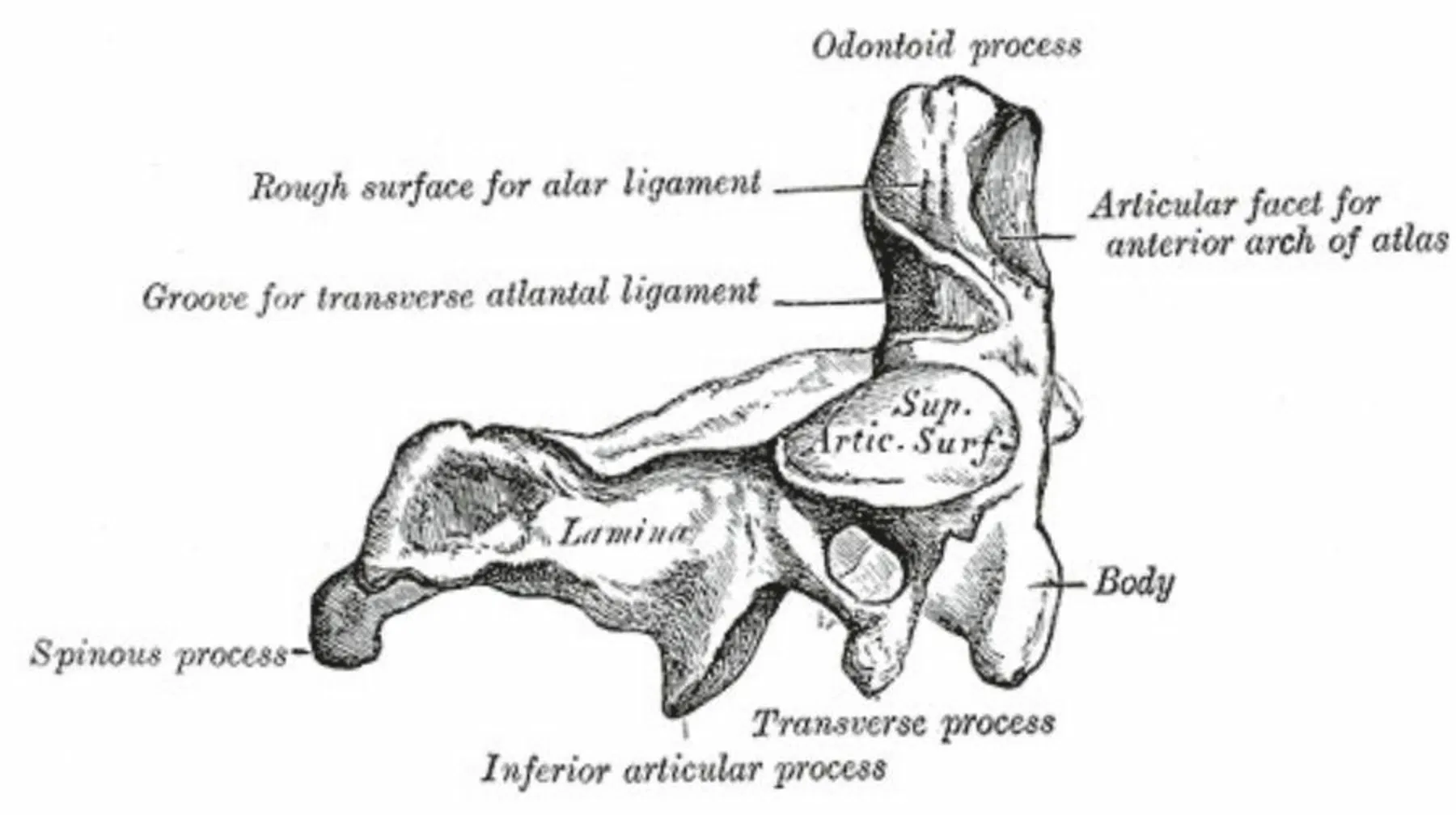
The Axis Bone
Exploring the Unique Causes of Headaches in Denver and How Chiropractic Care Provides Relief
The axis bone is the second vertebra in your cervical spine, and is critical in the movement of the head. The spine also consists of the thoracic spine, lumbar spine, sacrum, coccyx, and the intervertebral discs that interconnect the vertebrae. We’ll focus on the axis, or c2 vertebra here.
What is the function of atlas and axis? The atlas and axis form synovial joints that serve multiple functions , including the stability, rotation, flexion, and extension of the head and neck.
Misalignment of the axis bone can cause chronic headaches, neck pain, vertigo, and possibly even Meniere’s syndrome. Upper cervical chiropractic adjustment is an effective treatment for C2 misalignment.
If you’re worried about axis alignment, schedule an appointment with a qualified chiropractor who specializes in the upper spine.
What is the axis bone?
The axis bone is the second cervical vertebra in your vertebral column, or spine. With the atlas bone (C1) it forms the pivot joint that allows your head to rotate.
This important bone has many names:
- Axis
- Epistropheus
- Vertebra cervicalis II
- C2 vertebra
- Upper cervical spine (refers to both C1 and C2)
Why is it called the axis bone? The axis bone gets its name from the Latin word for “axle” which refers to a rod through the center of a wheel. The axis is instrumental in the rotation of the atlas bone and the head.
Is the axis C1 or C2? The axis bone refers to the second vertebra in the human anatomy, also called the C2. The C1 is your atlas .
Let’s explore the major features of the axis bone.
The vertebral body of the axis is the part which connects to the first cervical vertebra (C1) above and the C3 below. It is smaller than other vertebrae’s bodies. Also called the centrum, this cylindrical mass is located on the anterior surface (front side) of the vertebra.
The anterior longitudinal ligament attaches to the front of the body of the axis, but the posterior longitudinal ligament attaches to the back of the lower centrum.
The most unique feature of the axis bone is the dens, which protrudes upwards and acts as a stabilizing axle for the atlas bone and the head to rotate. The dens forms a pivot joint with the anterior arch of the atlas bone. Apical ligaments and alar ligaments connect the dens to the occipital bone.
This protrusion goes by several names:
- Dens
- Dens axis (literally “tooth of the axis”)
- Odontoid process
- Peg
The vertebral foramen is the large opening at the center of the axis bone which lets the spinal cord pass through. The axis’s foramen is smaller than the atlas’s.


The spinous process is a small projection backwards from the articulation of the two laminae of the axis’s vertebral arch. This process is where ligaments and muscles which move the head or neck may attach. The spinous process is bifid — or, naturally cleft into two segments.
The superior articular facets of the axis bone join with the inferior articular facets of the atlas bone to form the lateral atlantoaxial joints. Some sources refer to these as processes or surfaces instead of facets.
- The superior articular facets are convex surfaces that make head rotation possible, as well as articulation with occipital condyles. The superior articular processes allow one lateral mass to glide forward while another glides backward. This motion permits the C1 to rotate around the dens of the C2.
- Inferior articular facets are flat surfaces which face downward from the vertebral arch and touch the C3 below.
At the atlantoaxial joint, the axis’s spinal nerve exits the spinal cord through a small opening in the bone above the axis.
The transverse processes are below the superior articular facet, and they project laterally (to the side), ending in a single tubercle. This part of the axis is where certain head and neck muscles can attach.
The transverse foramen is a small opening in the transverse process which allows the vertebral artery and vein to pass through.
C1 & C2 Misalignment
The upper cervical spine consists of the atlas (C1) and axis (C2). When the C1 and C2 are misaligned, health complications follow. You should seek chiropractic treatment that includes x-ray diagnostics if you are experiencing C1 and C2 misalignment.
Upper cervical misalignment may contribute to multiple health problems, some of which may surprise you. Chiropractic adjustment can fix these health problems:
- Neck pain
- Chest pain (more common with thoracic vertebrae misalignment)
- Back pain (more common with lumbar vertebrae misalignment or muscle tension)
- Migraines
- Headaches
- Post-concussion syndrome
- Vertigo
- Meniere’s disease
- Fibromyalgia
- Chronic fatigue
- Autoimmunity
- High blood pressure
- TMJ disorders (jaw soreness)
- Sleep disturbances
- Trouble breathing
- Muscle weakness
- Sciatica
When to Get an Adjustment
You should get a chiropractic adjustment if you experience any of the following symptoms:
- Chronic neck pain
- Chronic headache or migraine
- Vertigo or cervical instability
- Trouble standing up or sitting down
- Constant jaw pain
- Noticeable spinal abnormalities
Schedule an appointment with Dr. Ty Carzoli at Denver Upper Cervical Chiropractic in Denver, Colorado. He is qualified to adjust the whole spine, but Dr. Ty has found that upper cervical spine adjustments alone can often treat health conditions. You can set up an appointment online or call us at 303-955-8270.
Sources:
- Korabelnikova, E. A., Danilov, A. B., Danilov, A. B., Vorobyeva, Y. D., Latysheva, N. V., & Artemenko, A. R. (2020). Sleep disorders and headache: A review of correlation and mutual influence. Pain and therapy , 9 (2), 411-425. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7648824/
- Elizagaray-Garcia, I., Beltran-Alacreu, H., Angulo-Díaz, S., Garrigos-Pedron, M., & Gil-Martinez, A. (2020). Chronic primary headache subjects have greater forward head posture than asymptomatic and episodic primary headache sufferers: Systematic review and meta-analysis. Pain medicine , 21 (10), 2465-2480. Full text: https://www.researchgate.net/profile/Ignacio-Elizagaray-Garcia-2/publication/345144818_Chronic_Primary_Headache_Subjects_Have_Greater_Forward_Head_Posture_than_Asymptomatic_and_Episodic_Primary_Headache_Sufferers_Systematic_Review_and_Meta-analysis/links/61c44cd7c99c4b37eb1878af/Chronic-Primary-Headache-Subjects-Have-Greater-Forward-Head-Posture-than-Asymptomatic-and-Episodic-Primary-Headache-Sufferers-Systematic-Review-and-Meta-analysis.pdf
- Fischer, M. A., & Jan, A. (2019). Medication-overuse headache. Full text: https://www.ncbi.nlm.nih.gov/books/NBK538150/
- Jovel, C. E., & Mejía, F. S. (2017). Caffeine and headache: specific remarks. Neurología (English Edition) , 32 (6), 394-398. Full text: https://www.sciencedirect.com/science/article/pii/S2173580817300858
- Leung, A. (2020). Addressing chronic persistent headaches after MTBI as a neuropathic pain state. The Journal of Headache and Pain , 21 (1), 77. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7304149/
- Kaur, A., & Singh, A. (2013). Clinical study of headache in relation to sinusitis and its management. Journal of Medicine and Life , 6 (4), 389. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3973877/
- Kikkeri, N. S., & Nagalli, S. (2022). Migraine with aura. In StatPearls [Internet]. StatPearls Publishing. Full text: https://www.ncbi.nlm.nih.gov/books/NBK554611/
- Ruschel, M. A. P., & De Jesus, O. (2023). Migraine headache. In StatPearls [Internet]. StatPearls Publishing. Full text: https://www.ncbi.nlm.nih.gov/books/NBK560787/
- Al Khalili, Y., & Chopra, P. (2020). Hypnic Headache. Full text: https://www.ncbi.nlm.nih.gov/books/NBK557598/
- Arca, K. N., & Halker Singh, R. B. (2019). The hypertensive headache: a review. Current pain and headache reports , 23 , 1-8. Full text: https://www.iranheadache.ir/wp-content/uploads/2020/04/The-Hypertensive-Headache-a-Review.pdf
- Jersey, A. M., & Foster, D. M. (2018). Cerebral aneurysm. Full text: https://www.ncbi.nlm.nih.gov/books/NBK507902/
- Vernon, H., Borody, C., Harris, G., Muir, B., Goldin, J., & Dinulos, M. (2015). A randomized pragmatic clinical trial of chiropractic care for headaches with and without a self-acupressure pillow. Journal of manipulative and physiological therapeutics , 38 (9), 637-643. Abstract: https://pubmed.ncbi.nlm.nih.gov/26548737/
- Al Khalili, Y., Ly, N., & Murphy, P. B. (2018). Cervicogenic headache. Full text: https://www.ncbi.nlm.nih.gov/books/NBK507862/
- Urits, I., Patel, M., Putz, M. E., Monteferrante, N. R., Nguyen, D., An, D., … & Viswanath, O. (2020). Acupuncture and its role in the treatment of migraine headaches. Neurology and therapy , 9 , 375-394. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7606388/
- Jimenez, M. P., DeVille, N. V., Elliott, E. G., Schiff, J. E., Wilt, G. E., Hart, J. E., & James, P. (2021). Associations between nature exposure and health: a review of the evidence. International Journal of Environmental Research and Public Health , 18 (9), 4790. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8125471/
The post The Axis Bonea ppeared first on Denver Upper Cervical Chiropractic.
© 2026 Denver Upper Cervical Chiropractic